As the rates of cancer continue to increase, largely because of early detection and diagnosis, the number of women looking into preserving their fertility is also on the rise.
It’s estimated that more than 500,000 women between the ages of 20 and 45 are diagnosed with cancer every year. The good news is that due to early screening, a lot of these women have a 5-year survival rate above 80 percent. But in looking towards survival, many women also begin to wonder if they’ll be able to have children after they finish treatment.
Standard therapy for many kinds of cancer includes things like surgery, chemotherapy and radiation – all of which can affect a woman’s reproductive organs – especially her ovaries. There are some chemotherapy drugs, such as alkylating agents, that, while very effective in killing cancer cells, can also have quite a toxic effect on ovarian tissue. Abdominal pelvic radiation can interrupt normal menstruation and affect uterine function.
While it may seem hard to think about days, weeks, months or years from now while you’re in the fight of your life, if having children is important to you, you should talk to your doctor about how treatment may affect your fertility and what your options may be for preserving it.
Freezing your eggs: This option has been gaining a lot of popularity over the past few years both in cancer patients and women who are just looking to start a family later in life. It includes stimulating the ovaries, harvesting eggs and freezing them for fertilization at a later date.
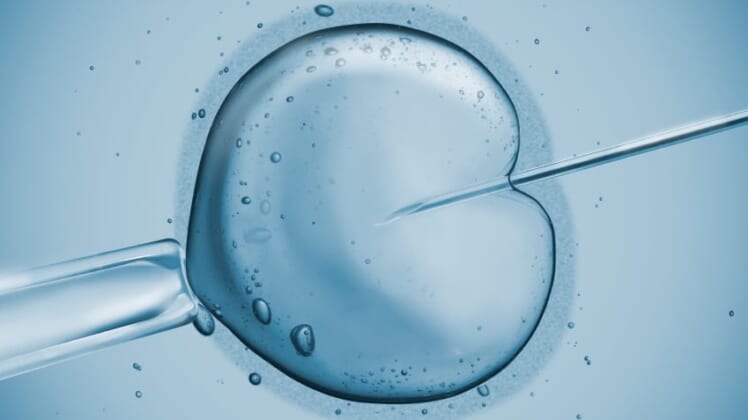
Embryo banking: This involves ovarian stimulation, egg retrieval and fertilization of the egg. The embryo is then cryogenically frozen to preserve it for later implantation, completing the in vitro fertilization (IVF) cycle. This is a popular option because the survival rate of those embryos is about 95 percent and depending on the age of the patient they are implanted into, has a live birth rate of about 42 percent.
Ovarian tissue banking: While still in the experimental stage, this involves surgical removal of part of the ovary and subsequent transplantation, with the goal, of course, to restore ovarian function after treatment.
Ovarian transposition: This is done before treatment starts to surgically reposition the ovaries away from the radiation field.
Donor eggs and embryos are also an option for some women after completing treatment. The key is to understand what kind of cancer you have and, especially for breast cancer patients, knowing whether or not your cancer is hormonally sensitive — which would definitely have an impact on future pregnancies and survival.
My advice is to explore some of these options. This can be done through a combination of talking to your oncologist and to a well-certified reproductive endocrinologist, in order to see which option may work best for you.
