A lot of parents ask me if they should bank their child’s umbilical cord blood in order to save the stem cells. While the practice of storing cord blood has been around for many years, there’s still a lot of confusion over the benefits of doing it.
Now, here are some facts: The blood inside the cord blood and the placenta is full of fetal stem cells that are unique to the child and have the potential for transplantation event of a medical crisis. Typical cord blood transplants are performed in cases of childhood cancers where there’s a need to replenish some of the cellular activity in the infant’s bone marrow so that they can thrive and function normally after treatment.
Approximately 1 in 10,000 kids are afflicted with childhood cancers, so you could see why many parents may believe that storing their child’s cord blood may not be important, and why there are cord blood banks available that parents do have access to in emergency situations. The problem then becomes, of course, finding the perfect match.
But there’s another side to banking cord blood that involves stem cell technology— and that is cellular re-engineering. This is a field that is gathering a lot of attention because we already have enough information to successfully re-engineer and culture stem cells so that they transform themselves into other tissues. The perfect example of this practice is how stem cell technology is being utilized today for the formation of cartilage and skin. Researchers at Wake Forest University have even used stem cells for the re-engineering of urinary bladders and the transplantation of those bladders in patients who did not have them at birth.
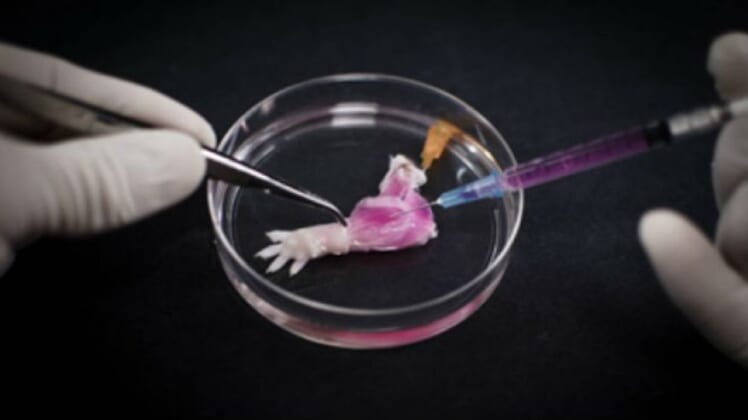
And now, we see this experiment being conducted at Massachusetts General Hospital, where, again, doctors used bioengineering cells to regrow the leg of a rat. Researchers drew living cells from a donor organ, stripped them with a detergent solution, and repopulated the components of the limb— including bone, cartilage, ligaments and nerves— with progenitor cells that matched the limb to create a structure called the matrix. The team was able to remove cellular materials from the deceased rats and save the primary vasculature and nerve matrix.
They then created a cell-free matrix and injected muscle progenitors into the matrix sheaths that indicate each muscle’s position, designing a fully functional bioartificial limb. The study authors noted in a press release that 1.5 million Americans have lost a limb, and that their method could replace sometimes-burdensome prosthetic technology.
So the bottom line is this: There will be many diseases and conditions that will be treated by stem cell re-engineering that might completely eradicate whatever problem is in question. Not only could this impact the re-engineering of body parts or organs, but stem cell technology will also be able to create unique opportunities to doctors to evaluate best practices when it comes to medication dosages or specific medications to treat disease.
And this will have a fundamental impact on improving outcomes. So I am bullish in trying to preserve umbilical cord blood, and I think that, as the technology improves, even the cause of banking umbilical cord blood will be more accessible to patients— and it will create a safeguard for those individuals.
